Osteotomies of the proximal femur are performed to realign the hip joint or the femur for proper function. It involves dividing the bone, correcting the deformity, and stabilizing the bone fragments in the new position to promote quick healing. Femoral osteotomy is considered a major operation that takes 1–2 hours under adequate anesthesia, involves moderate amount of blood loss, hospitalization for 2–3 days, and limited weight bearing with a walker or crutches for 6 weeks. Infection and delayed healing can occur needing more surgery. The plate and screws used to fix the bones in growing children are usually removed after adequate healing the bones.
Rotational Osteotomy
Femoral rotational deformity can be from head tilt, neck shaft version, or torsion in the shaft. Head tilt as in a SCFE is ideally corrected with a sub capital osteotomy, neck version with inter trochanteric rotational osteotomy plus greater trochanter (GT) transfer to realign the abductor insertion, and shaft torsion with a shaft osteotomy. Rotation osteotomy distal to the GT performed without GT optimization may not always influence the hip and may just change the foot progression angle.
A rotational osteotomy of the femur can be done at any level, but the more distal osteotomy has less effect on the hip. I aim to do it just below the lesser trochanter when using a blade plate and more distal when using a nail. Healing has not been an issue with minimal stripping, low heat producing osteotomy, good contact of the fragments, and stable fixation. Different than a traumatic ST fracture which requires a lot of energy, strips soft tissues, and difficult to reduce and fix well.
Percutaneous Technique (IM Nail)
The osteotomy is performed with open incision for plate fixation and is percutaneous for intramedullary nail fixation. Reaming after performing the osteotomy theoretically decreases embolism and pushes bone graft into the osteotomy site. Avoids the need for additional venting of the canal.
The amount of rotational correction can be estimated clinically by inserting half pins away from the nail path in the proximal and distal femur before completing the osteotomy and dialing in the correction based on the pin position afterwards. The proximal pin is placed medially just proximal to the lesser trochanter from straight anterior to posterior and the distal pin is placed into the lateral femoral condyle in the mid lateral plane. The two pins are at 90 degree angle to each other. The final correction is confirmed by examining the hip rotation after fixation of both fragments with screws.
The sequence was pin placement, proximal canal entry, percutaneous osteotomy, reaming over a guidewire, nail just across the osteotomy, rotate and compress the osteotomy, seat and lock the nail.
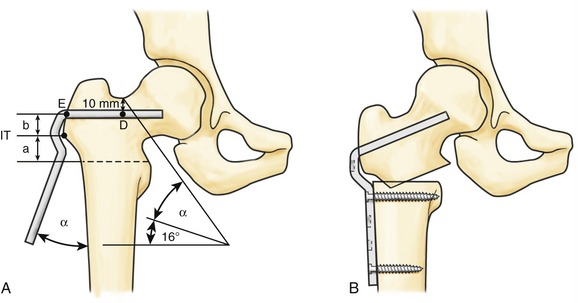
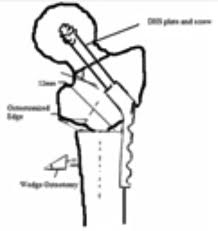
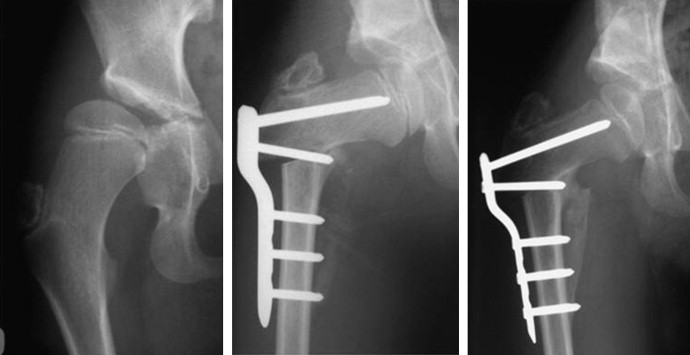
Valgus Osteotomy
Valgus osteotomy of the hip is better done below the lesser trochanter with lateral translation of the distal fragment and varus above the lesser trochanter with medial translation.
Femoral Neck Nonunion & Valgus Osteotomy
The ideal treatment should restore neck length, healing and normal hip function. A biologic bone block plus fixation in the nonunion site will be the best if available.
| Option | Details |
|---|---|
| Direct bone grafting | Not commonly done or required — donor site morbidity, extra dissection, time, cost |
| Fibular strut grafting | Commonly done — restores neck bone mass and length — donor site morbidity, extra work, needs spacing with hardware and additional valgus osteotomy |
| Valgus osteotomy | Most commonly done — flattens the fx line, increases compression, stimulates healing — decreases abductor lever arm and pelvic width, increases hip stresses, FIR, leg length, abductor resting length |
Normal hip function requires:
- Neck angle and offset — to decrease impingement
- Neck length / lateral offset — abductor lever arm, pelvis width, ischial impingement, joint forces
- Greater trochanter height — abductor resting length, joint stresses, GT impingement
Clinical Scenarios
- 1 If closed reduction with traction restores acceptable NSA, version, and neck length — stabilize the head on the neck, fix with sliding device, add valgus osteotomy (fibula is an option)
- 2 Open reduce the fracture if needed with or without bone grafting — fix plus valgus osteotomy
- 3 Neck resorbed — accept coxa breva, increase neck length with bone graft — sliding implant if bone graft is structurally sound — if not, bridging fixation across the nonunion and valgus osteotomy
Effects of Valgus at Any Level
| Valgus Level | Characteristics |
|---|---|
| Medial to intertrochanteric line | Minimizes GT height changes and medialization of femoral shaft, but increases instability from capsulotomy — opening wedge lengthens neck but slows healing — closing wedge shortens neck and increases instability — no need for a plate |
| Through the Greater Trochanter | Only closing wedge possible — good cancellous surfaces bleeding into osteotomy site — can put good bone into nonunion site without capsulotomy — fixation not strong enough to avoid external support — cable around GT & LT can avoid bracing |
| Just above LT | Opening wedge tensions iliopsoas and restricts lateral translation — less translation required to restore mechanical axis — easier to translate with closing wedge — plate fixation indicated |
| Below LT | Needs maximum translation to restore axes — less bone contact — medial prominence of lesser trochanter can impinge against ischium — needs strong fixation |
Solutions for Side Effects
- Foveal impingement or lateral instability — corrected by PAO or second stage varus osteotomy
- Neck length — increased with true or relative neck lengthening
- Medialization of femur — corrected with lateral translation of the shaft
- Abductor lever arm — increased with varus or lateral transfer of GT
- Abductor resting length — shortened with proximal transfer of GT
- LT impingement — relieved with LT excision
- Leg length — shortened by removing some medial cortex
Principles & Technique (Valgus)
Femoral neck nonunion fixation is done either with an implant that allows sliding and dynamic compression of the nonunion site or bridging implant to maintain neck length. Dynamic compression is achieved by placing the implant along the neck axis. Bridging screws need not be along the neck axis but they need to have good fixation into the head.
Subtrochanteric valgus osteotomy requires strong fixation in the proximal fragment and distal fragment with good compression between the two fragments. Strong fixation into a short proximal fragment is best achieved with a fixed angle device. The angle of the plate is less important in isolated subtrochanteric osteotomy fixation. Even a 90 degree blade plate can be used to get 145 NSA by inserting the blade in 55 degrees of varus into the proximal fragment. Even an IM rod can be used by reaming the proximal canal to align with the distal canal after correction.
The ideal implant to fix the head well along the neck axis and get a 145 neck shaft angle is a 145 degree blade plate or DHS. The ideal bridging fixation is a 145 degree locking plate. Any other angle will compromise the alignment or fixation.
Blade plate chisel needs to be inserted correctly in two planes and is harder to revise or adjust due to the bigger tract it makes. Locking plates are easier with adjustment of the sagittal plane with the second screw. A single angle plate will get lateral translation automatically, while the top bend needs to be left proud over the GT to get the same translation with a double angled plate. Lateral translation can be increased by leaving either plate proud at the GT. Appropriate translation aligns the femoral shaft with the piriformis fossa and limb mechanical axis to pass through the center of the knee.
Simplified Step-by-Step (Valgus)
- 1 Varus above GT, valgus below GT
- 2 Varus translate medially, valgus laterally, flexion anteriorly, extension posteriorly till the shaft lines up with the piriformis fossa
- 3 Select a fixed angle implant with the angle closest to the target neck shaft angle
- 4 Decide where the blade or locking screws go into the proximal fragment — put them in a way that when the plate is reduced to the shaft after the osteotomy, you get your NSA and flexion/extension — for example, if you want 145 NSA, put the blade in the center of the neck if a 145 plate is available — if you have a 120 plate, put it in 25 degrees of varus to get 145
- 5 Valgus plate can be fixed fully to the proximal fragment before performing the osteotomy; varus after completing the osteotomy and displacing the bone fragments
- 6 Consider cabling Gluteus medius tendon to the plate for big valgus corrections to protect the GT and prevent the plate from cutting out
- 7 Mark the rotation before osteotomy or decide on optimal rotation based on hip motion after provisional fixation of the plate to the shaft
- 8 Fix the plate to proximal fragment adjusting the depth of insertion to the desired translation — reduce plate to shaft, verify correction, adjust translation and rotation — compress the osteotomy by manual loading, dynamic screw compression, or lagging the bone to plate from distal to proximal
Practical Issues
- Availability of full hardware — hip plates from Synthes are expensive; there are equivalent implants from local manufacturers
- Calculation of NSA and estimation of desired correction can be tricky with long-standing pathologies and confounding torsional malalignment
- Soft tissue factors — scarring from previous surgeries and infectious etiology
Reconstruction Goal
Put the best cartilage to bear weight, stable joint, impingement-free motion, and good abductor function. ATD, leg length, and cosmesis are dealt with separately if needed without compromising the primary goal.
Varus Deformity Correction
- Head varus like a SCFE — neck osteotomy is ideal; distal osteotomy with proper translation is acceptable
- Short neck and high GT — GT transfer or RNL to also increase FIR
- Varus at the neck shaft — valgus peritrochanteric osteotomy
Effects of Varus at Any Level
| Varus Level | Characteristics |
|---|---|
| Medial to intertrochanteric line | Minimizes GT height change — correct level for caput valgum correction, but more complicated to perform and heal — opening wedge lengthens neck but slows healing — closing wedge shortens neck and increases instability — no need for a plate |
| Just above LT | Opening wedge minimizes shortening — less translation required — decreases FIR and increases risk of impingement — GT becomes very prominent laterally — plate fixation necessary |
| Below LT | Needs maximum translation to restore axes — less bone contact — medial capsule and iliopsoas resist varus correction — needs strong fixation — distal end of proximal fragment and plate become very prominent unless plate is sunk deeper |
Solutions for Varus Side Effects
- GT height and FIR — corrected with RNL
- Neck length — decreased with neck shortening
- Lateralization of femur — corrected with medial translation of the plate and shaft
Step-by-Step (Varus)
- 1 Varus above GT, valgus below GT
- 2 Translate medially for varus, laterally for valgus, anteriorly for flexion, posteriorly for extension until the shaft lines up with the piriformis fossa
- 3 Select a fixed angle implant with the angle closest to the target neck shaft angle
- 4 Decide where the blade or locking screws go into the proximal fragment so that when the plate is fixed and reduced to the shaft, you achieve your NSA and flexion/extension — for 120 NSA with a 120 plate, put chisel in center of neck — with a 110 plate, put it in 10 degrees of valgus to get 120
- 5 Varus plate can be fixed to the proximal fragment only after performing the osteotomy — ensure the chisel is loose for easy withdrawal after the osteotomy
- 6 Mark rotation before osteotomy or decide based on hip motion after provisional fixation
- 7 Fix the plate to the proximal fragment adjusting depth of insertion for desired translation — removing the lateral cortex allows deeper seating of the plate
- 8 Reduce plate to shaft, verify correction, adjust translation and rotation — compress the osteotomy by manual loading, dynamic screw compression, or lagging bone to plate from distal to proximal
Key Principle
Varus or valgus osteotomies can be done with any implant if the correction is obtained first and the implant is fixed to both fragments to hold that correction.
